 1 Hemodynamically unstable patients with AFl should receive synchronized electrical cardioversion. AFL was misdiagnosed more often than AF, with atypical more often than typical AFL. 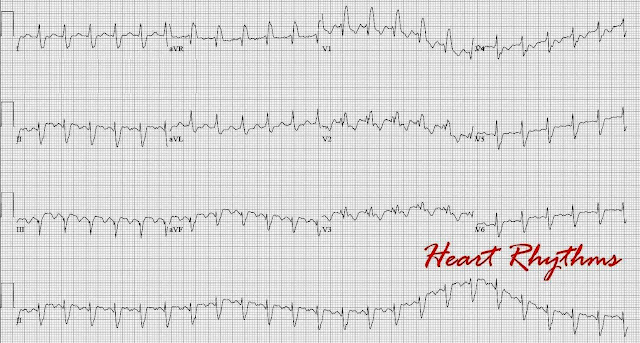
4 If rhythm identification is unclear and the patient is stable, adenosine or Valsalva maneuver may be employed to slow conduction through the AV node such that the atrial flutter waves are more readily apparent. ECGs, interpreted as AF or AFL by internists, are often misdiagnosed. The initial treatment for AFl focuses on rate control of the ventricular response with AV nodal blocking agents such as beta-blockers and calcium channel blockers. Electrophysiological studies have defined multiple mechanisms of tachycardia, both re-entrant and focal, with varying ECG morphologies and rates, authenticated by the results of catheter ablation of the focal triggers or critical isthmuses of re-entry circuits. Atrial flutter can described as typical (type I) or atypical (type II) based on the anatomic location from which it originates. Atypical flutter occurs outside the CTI around areas of atrial scar tissue. Common symptoms of AFl include palpitations, light-headedness, fatigue, presyncope, mild shortness of breath, and possibly chest pain or hypotension. 1 Risk factors for AFl include presence of heart failure, chronic obstructive pulmonary disease, antiarrhythmic medications, thyrotoxicosis, pulmonary embolism, prior cardiac surgery or prior atrial ablation. Your heart’s chambers can’t fill with blood fast. Atrial flutter is like an assembly line with the speed set too fast at the line’s first station. This causes your lower chambers to beat fast as a response, commonly as fast as 150 beats a minute or more. 300 bpm (200-400 bpm) with a heart rate typically ca. The underlying mechanism of type II AFl is unclear. Atrial flutter can make your heart’s upper chambers beat 250 to 350 times a minute. Afib and atypical Aflutter requires more expertise and radiofrequency ablation has lower success rate. 3 The ECG in atypical (type II) AFl is characterized by upright F waves in leads II, III, aVF, and V 6 and by biphasic F waves in leads I, aVL, and V 1. 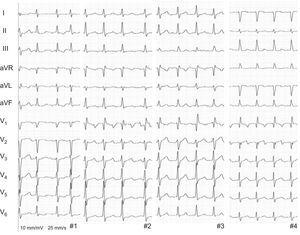
2 Type I AFl is most commonly caused by the presence of a macro-reentrant circuit in the right atrium that includes a small strip of tissue between the inferior vena cava and the tricuspid annulus known as the cavotricuspid isthmus. 1 The ECG in type I (typical) AFl is characterized by an inverted sawtooth flutter (F) wave pattern in the inferior leads II, III, and aVF, low amplitude biphasic F waves in leads I and aVL, an upright F wave in precordial lead V 1, and an inverted F wave in lead V 6. Typical atrial flutter represents at least 90 of all flutters, and has usually a counterclockwise pattern. Atypical atrial flutters are composed by non-isthmus-dependent right atrial flutter and left atrial flutter. 
Atrial flutter (AFl) is a cardiac dysrhythmia characterized by rapid and regular depolarization of the atria that appears as a sawtooth pattern on the electrocardiogram (ECG) and is categorized into type I (typical) and type II (atypical) AFl. Typical atrial flutter comprises counterclockwise and clockwise isthmus-dependent atrial flutter located within the right atrium. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
